Understanding career motivation for medical specialization: the roles of perceived benefits, barriers, and facilitating conditions
Main Article Content
Abstract
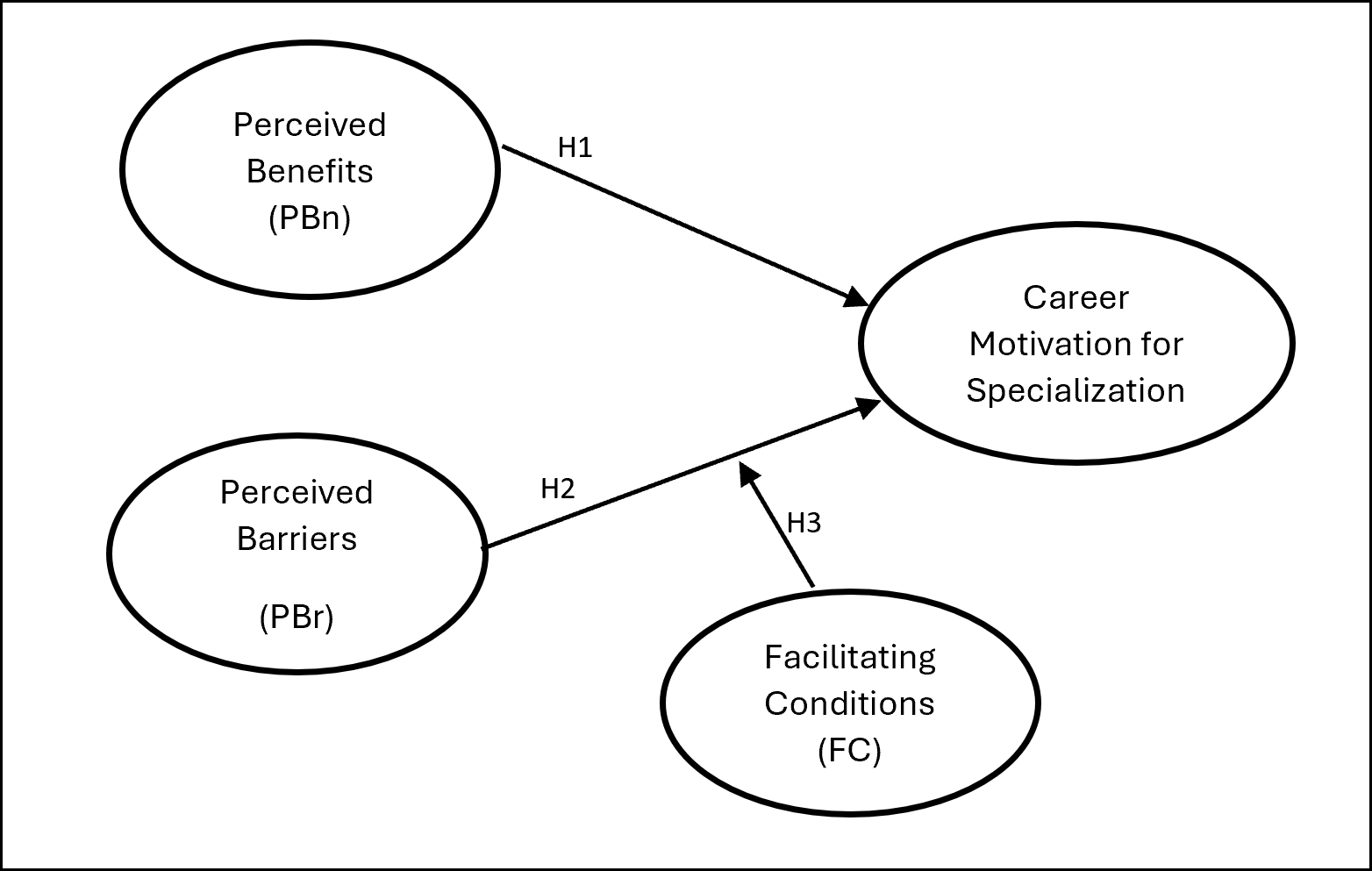
Specialized medical care is crucial for addressing the increasing prevalence of chronic and non-communicable diseases in Malaysia. However, there is still a shortage of medical specialists, which remains a challenge to be solved if medical officers lack the motivation to pursue a specialization. This lack of motivation is influenced by various contextual factors. This study applies the London’s Career Motivation Theory to investigate the interplay between perceived benefits, perceived barriers, facilitating conditions, and career motivation for specialization among medical officers. Partial Least Squares Structural Equation Modelling was used within a quantitative approach to examine the proposed hypotheses. Data were collected from medical officers in healthcare clinics and hospitals across various states, and 309 valid responses were obtained. The findings reveal a positive association between perceived benefits and career motivation, while perceived barriers correlate negatively with career motivation. Additionally, facilitative conditions moderate the relationship between perceived barriers and career motivation for specialization. These results hold significant implications for healthcare organizations and policymakers.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
References
Abdulrahman, M., Farooq, M. M., Kharmiri, A. A., Marzooqi, F. A., & Frederick, C. (2018). Burnout and depression among medical residents in the United Arab Emirates: A multicenter study. Journal of Family Medicine and Primary Care, 7(2), 435. https://doi.org/10.4103/jfmpc.jfmpc_199_17
Abdulrahman, M., Makki, M., Shaaban, S., Shamsi, M. A., Venkatramana, M., Sulaiman, N., Sami, M. M., Abdelmannan, D., Salih, A. M., & AlShaer, L. (2017). Specialty preferences and motivating factors: A national survey on medical students from five UAE medical schools. PubMed, 29(3), 231–243. https://doi.org/10.4103/13576283.204225
Al-Khaldi, Y. (2023). Research in family medicine: Contribution, priorities, and barriers in Saudi Arabia. Journal of Family and Community Medicine, 30(2), 137. https://doi.org/10.4103/jfcm.jfcm_388_22
Alqanatish, J., Yazeed, A., Amr, A., Malek, A., & Masud, N. (2020). Factors affecting the selection of future sub-specialties among paediatric residents in Saudi residency training during the 2016–2017 academic year. Health Professions Education, 6(1), 115–121. https://doi.org/10.1016/j.hpe.2019.05.005
Anderson, J. C., & Gerbing, D. W. (1988). Structural equation modeling in practice: A review and recommended two-step approach. Psychological Bulletin, 103(3), 411–423. https://doi.org/10.1037/0033-2909.103.3.411
Bailey, N., Mandeville, K. L., Rhodes, T., Mipando, M., & Muula, A. S. (2012). Postgraduate career intentions of medical students and recent graduates in Malawi: A qualitative interview study. BMC Medical Education, 12(1). https://doi.org/10.1186/1472-6920-12-87
Cameron, J. K., Bilszta, J., Reid, K., & Briggs, C. (2019). Motivations & experiences of postgraduate anatomy training. MedEdPublish, 8, 62. https://doi.org/10.15694/mep.2019.000062.1
Chawla, J., Arora, M. K., Datta, K. K., Singh, S. K., & Arora, A. K. (2018). Factors affecting postgraduate planning among undergraduate medical students: A prospective observational study from India. Southeast Asian Journal of Medical Education, 12(2), 35. https://doi.org/10.4038/seajme.v12i2.50
Chefchaouni, A. C., Bennani, I., Kartouti, A. E., Chaouir, S., Elalaoui, Y., & Rahali, Y. (2024). The quest for specialization among health professionals at Moroccan university hospitals: A study of motivations and influences. Le Pharmacien Clinicien. https://doi.org/10.1016/j.phacli.2023.12.002
Chin, W. W. (1998). Issues and opinion on structural equation modeling. Management Information Systems Quarterly, 22(1), 7–16. https://doi.org/10.5555/290231.290235
Ferreira, T., Collins, A., Feng, O. Y., Samworth, R. J., & Horvath, R. (2023). Career intentions of medical students in the UK: A national, cross-sectional study (AIMS study). BMJ Open, 13(9), e075598. https://doi.org/10.1136/bmjopen-2023-075598
Franke, G. R., & Sarstedt, M. (2019). Heuristics versus statistics in discriminant validity testing: A comparison of four procedures. Internet Research, 29(3), 430–447. https://doi.org/10.1108/intr-12-2017-0515
Grzeda, M., & Prince, J. B. (1997). Career motivation measures: A test of convergent and discriminant validity. The International Journal of Human Resource Management, 8(2), 172–196. https://doi.org/10.1080/09585199700000047
Hair, J. F., Thomas, G., Hult, M., Ringle, C. M., & Sarstedt, M. (2022). A primer on partial least squares structural equation modeling (3rd ed.). Sage.
Hammadi, W. A., Hammadi, H. A., & El-Shereef, E. A. (2020). Study of future specialty career choice among female medical students in Medical College, Taif University, Saudi Arabia. International Journal of Medical Research & Health Sciences, 9(9), 40–48.
Hames, K., Patlas, M. N., & Duszak, R. (2018). Barriers to resident research in radiology: A Canadian perspective. Canadian Association of Radiologists Journal, 69(3), 260–265. https://doi.org/10.1016/j.carj.2018.03.006
Haruta, J., Ozone, S., & Hamano, J. (2020). Doctors’ professional identity and socialization from medical students to staff doctors in Japan: Narrative analysis in qualitative research from a family physician perspective. BMJ Open, 10(7), e035300. https://doi.org/10.1136/bmjopen-2019-035300
Khalid, A., & Rathore, K. (2018). Mediating effect of work-life balance on work motivation of postgraduate trainee doctors in public sector hospitals: Evidence from Pakistan. Pakistan Economic and Social Review, 56(1). https://www.jstor.org/stable/26616734
Khamees, A., Awadi, S., Sharie, S. A., Faiyoumi, B. A., Alzubi, E. M., Hailat, L., & Al-Keder, B. (2022). Factors affecting medical students’ decision in choosing a future career specialty: A cross-sectional study. Annals of Medicine and Surgery, 74. https://doi.org/10.1016/j.amsu.2022.103305
Klifto, K. M., Payne, R. M., Siotos, C., Lifchez, S. D., Cooney, D. S., Broderick, K. P., Aliu, O., Manahan, M. A., Rosson, G. D., & Cooney, C. M. (2020). Women continue to be underrepresented in surgery: A study of AMA and ACGME data from 2000 to 2016. Journal of Surgical Education, 77(2), 362–368. https://doi.org/10.1016/j.jsurg.2019.10.001
Ladha, F. A., Pettinato, A. M., & Perrin, A. E. (2022). Medical student residency preferences and motivational factors: A longitudinal, single-institution perspective. BMC Medical Education, 22(1). https://doi.org/10.1186/s12909-022-03244-7
Levaillant, M., Levaillant, L., Lerolle, N., Vallet, B., & Hamel-Broza, J. (2020). Factors influencing medical students’ choice of specialization: A gender-based systematic review. EClinicalMedicine, 28, 100589. https://doi.org/10.1016/j.eclinm.2020.100589
Li, W., & Sun, H. (2018). Specialist training and career intentions of international medical students coming from Asia and Africa. International Medical Student Education, 1(1), 1–8.
London, M. (1983). Toward a theory of career motivation. The Academy of Management Review, 8(4), 620–630. https://doi.org/10.2307/258263
Mahfouz, M., Althobaiti, Z. F., Alosaimi, S. G., Alghamdi, Y., Alharthi, H. E., Althobaiti, A. M., & Altowairqi, F. K. (2021). Specialty choice among final-year medical students at Taif University. The Saudi Journal of Health Systems Research, 1(3), 115–122. https://doi.org/10.1159/000517662
Malaysian Performance Unit. (2020). Malaysian health at a glance. Ministry of Health Malaysia. https://www.moh.gov.my/moh/penerbitan/MYHAAG2018.pdf
Mohamed, E. Y. (2022). Specialty preferences and factors affecting the choices of postgraduate specialty among undergraduate medical students. Pakistan Journal of Medical Sciences, 38(6), 103305. https://doi.org/10.12669/pjms.38.6.5571
Nadarajah, A., Shankar, P. R., Jayaraman, S., & Sreeramareddy, C. T. (2022). House officers’ specialist career choices and motivators for their choice: A sequential mixed-methods study from Malaysia. BMC Medical Education, 22(1). https://doi.org/10.1186/s12909-022-03845-2
Nair, S. C., Ibrahim, H., Almarzoqi, F., Alkhemeiri, A., & Sreedharan, J. (2019). Addressing research barriers and facilitators in medical residency. Journal of Family Medicine and Primary Care, 8(3), 1145–1150. https://doi.org/10.4103/jfmpc.jfmpc_38_19
Noe, R. A., Noe, A. W., & Bachhuber, J. A. (1990). An investigation of the correlates of career motivation. Journal of Vocational Behavior, 37(3), 340–356. https://doi.org/10.1016/0001-8791(90)90049-8
Ojo, E., Chirdan, O., Ajape, A., Agbo, S., Oguntola, A., Adejumo, A., & Babayo, U. (2014). Postgraduate surgical training in Nigeria: The trainees’ perspective. Nigerian Medical Journal, 55(4), 342. https://doi.org/10.4103/0300-1652.137227
Okunlola, A. I., Babalola, O. F., Okunlola, C. K., Salawu, A. I., Adeyemo, O. T., & Adebara, I. O. (2020). Determining factors for the choice of medical career among final-year medical students of a private university in Nigeria. Journal of the National Association of Resident Doctors of Nigeria, 29(2), 308. https://doi.org/10.4103/njm.njm_79_20
Saeed, I., Khan, N. F., Bari, A., & Khan, R. A. (2018). Factors contributing to the lack of interest in research activities among postgraduate medical students. Pakistan Journal of Medical Sciences, 34(4), 913–917. https://doi.org/10.12669/pjms.344.15411
Scanlan, G. M., Cleland, J., Walker, K., & Johnston, P. (2018). Does perceived organisational support influence career intentions? The qualitative stories shared by UK early career doctors. BMJ Open, 8(6), e022833. https://doi.org/10.1136/bmjopen-2018-022833
Sekaran, U., & Bougie, R. (2016). Research methods for business: A skill-building approach (7th ed.). http://103.227.140.9/handle/123456789/18302
Spooner, S., Pearson, E., Gibson, J., & Checkland, K. (2017). How do workplaces, working practices and colleagues affect UK doctors’ career decisions? A qualitative study of junior doctors’ career decision making in the UK. BMJ Open, 7(10), e018462. https://doi.org/10.1136/bmjopen-2017-018462
Sriram, V., & Bennett, S. (2020). Strengthening medical specialization policy in low-income and middle-income countries. BMJ Global Health, 5(2), e002053. https://doi.org/10.1136/bmjgh-2019-002053
Sullivan, B., McGrail, M., Gurney, T., & Martin, P. (2021). Barriers to getting into postgraduate specialty training for junior Australian doctors: An interview-based study. PLOS ONE, 16(10), e0258584. https://doi.org/10.1371/journal.pone.0258584
Tang, L., Yang, H., Mao, Z., Li, Q., & Li, S. (2022). The negative factors influencing the career intention of general practice trainees in eastern China: A qualitative study. BMC Medical Education, 22(1). https://doi.org/10.1186/s12909-022-03456-x
The Star. (2024). Let doctors decide if they need HLP to specialize, says MMA. The Star. https://www.thestar.com.my/news/nation/2024/02/06/let-doctors-decide-if-they-need-hlp-to-specialise-saysmma